
|
|
|
|
|
|
|

|
|
 |
|
|
|
|
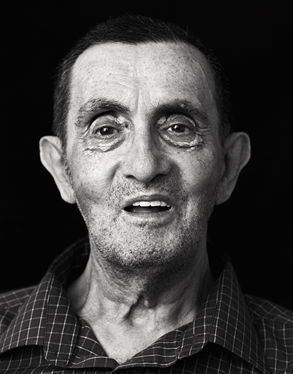
* It is the great leveller. And the last taboo. It brings down rich and poor alike. Hollywood gives it glamour; poets gild it with romance. Oscar Wilde even tried to make light of it. "My wallpaper and I are fighting a duel to the death. One or other of us has got to go," he muttered from a Parisian hotel, sipping his last champagne. Our tabloids mawkishly follow its path, too, through the spectacle of reality TV star Jade Goody and actors such as Farrah Fawcett and Patrick Swayze fighting their doomed battles with cancer. In our topsy-turvy world, you can experiment with drugs, sex, music, alter your body, aspire to billion-dollar empires from barrow-boy dreams, or immerse yourself in virtual worlds. But Death still terrifies – particularly in a society that is constantly on the move, increasingly individualised, its communities and traditional beliefs in upheaval. Yet according to a recent survey from theology think-tank Theos, we don't talk about death nearly enough. If we did, then maybe half of us would not fear it, says its director Paul Woolley: "Death today is handled very differently from the way it was in the past. For example, in the Victorian period, it was common practice for people when they had died to be kept in the home that they lived in, in an open coffin. Relatives paid their respects and would see a dead body, so death in terms of the frequency of it and people's day-to-day contact with it was higher and less removed." In Mexico, El Día de los Muertos ('Day of the Dead') sees families coming together to celebrate loved ones who have passed away, honoring the deceased using sugar skulls, marigolds, and the favorite foods and drinks of the departed. In more ancient cultures still, like the tribal clans in Papua New Guinea, ancestors are venerated and spirits take a daily part in peoples' lives. Yet it is not just our society that shies from mortality. Chinese emperors long sought the secret of eternal life, ingesting strange concoctions and minerals in an effort to stave off the inevitable (several are thought to have died as a result of poisoning from these 'elixirs'). Today the internet links a modern-day equivalent: Extropians, individuals dedicated to defeating death and prolonging life through scientific advance. One, a friend of mine, has paid £10,000 to have his head frozen when he dies. ("My insurance policy," he says, joking: "Hey, it's worth a shot!") Yet we still die. And there is a whole branch of medicine dedicated to the dying: palliative care. Palliative care aims to bring dignity and quality of life, through measures such as pain relief, to those with life-limiting and terminal conditions. Palliative care practitioners don't aim to "cure" – their goal is to prevent and relieve suffering. Many argue that the mainstream medical profession is still too focused on impersonal hospital care and prolonging life, even when it causes suffering to the patient (and their family). In the brilliant heat of a South African spring, I came across one of palliative care’s champions. Father Kieran Creagh ministered to the dying at the Leratong Hospice, just west of Pretoria, in a shanty town that had been wracked by inter-communal violence. HIV/AIDS had decimated this community. Creagh told me of his passionate belief in bringing dignity for the dying, many of whom were cast out by their own families and left to rot inside filthy, cloying shacks. He had seen the IRA murder two men on his very doorstep when he was just 14; in 2007 he was shot three times by robbers and had to be resuscitated on the operating table. "Seeing all the evil of The Troubles, I thought there had to be answer," he told me from the very courtyard where he had been shot. "People were dropping like flies here, too, of AIDS, young girls who'd done nothing wrong. I couldn't just stand and do nothing." The hospice he built now cares for hundreds of patients a year; not only that, it brings life – in the form of anti-retroviral drugs – to those who would otherwise die of their disease. Many other hospices took out food parcels to the poor and the sick; or like Leratong, provided clinics and creches where patients and their families could find respite from the desperate grind of their all-too-short lives. Creagh's passion got me thinking about the UK. Why do we run from death? Visiting British hospices, with help from its national federation, Help the Hospices, I saw the priceless work undertaken by countless volunteers (there are 100,000 of them up and down the country) helping bring dignity and love to those facing the end of their days. A quarter of a million people are cared for by these organisations every year, either in the hospice itself or in their own home (a large number of us wish to die in our own beds, research shows). All too often, though, the work of hospices is neglected. Few receive a penny from the Government, mostly relying on donations. In the UK, £1.3 million is spent on hospice care every day. Of this, only £397,000 comes from government sources, leaving hospices to raise another £903,000 per day. As I met individuals facing up to their own death, I learned, too, that the staff helping them talked very much about 'living with dying': we rarely just keel over (unlike Hollywood movies). There may be many months, and years, of scans, treatments, side effects and fears to deal with. Hospices will help through this journey. Often there can be remissions, too. In the course of this article I spoke on the phone with those who died before I could meet them; who died shortly after we had met; and those who also entered remission (from their disease) and are still with us today. We have recently passed the anniversary of the UK Government’s first ever End of Life Strategy (July 2008): a 10 year plan outlining how society should approach care for the terminally ill, allowing more choice and control over the way we end our lives. It included an extra £268m for palliative care. According to David Praill, chief executive of Help the Hospices: "The majority of hospice care is provided by local charities in people's own homes, and the chances of dying in your preferred location increases if you are being cared for by a local hospice," he said. If there was a common theme among the individuals I met on this final journey, it was that they were both unremarkable and at the same time most remarkable. Only two knew each other, Mandy and David, from their work on national palliative care committees. If there was another common trait they all shared, however, it was determination. Each had a commitment to charity (or in David’s case, politics), to do something for the future – even if they wouldn’t be around to see it. And most of all they were full of life! Humour and passion bubbled out of them, even at their lowest ebb. They were – they are – very ordinary yet inspirational individuals. I hope their messages, and my journey, serve to lift the dark veil on death. Just a little. For isn’t it time we acknowledge who and what we really are? As playwright Bertolt Brecht put it: “Do not fear death so much, but rather the inadequate life." * David David Hart, 69, Lambeth, London: Throat, Liver, Colon Cancer. David can hardly speak. The cancer has seen to that. It is eating away his throat. But from within his sunken face sparkle dark, humorous eyes. He may be slipping away to the disease which has twice revisited him, but David remains very much alive. “I’m supposed to be terminally ill,” he slurs, his voice a whisper. “Dying of cancer. Colon, liver ... throat,” he lists. “I’m not bothered with it,” he answers. “I’ve got good care, three carers, one of the poor buggers is in there right now [points to kitchen].” David is a journalist and lobbyist. Housing and issues around “dying well” concern him. He has lobbied against assisted suicide. He has a fierce, dry wit. The flat about him is small; hot. There are pictures of daughters, dead wives, friends and grandkids. One photo shows a jovial, fleshy man, round-faced: with a shock I realise this is the same figure in front of me now. A Burmese carer is present at all times. David is Jewish but for many years has been involved in the Free Burma campaign. He has cared for and buried two wives; seen close up what terminal disease can do. "I was married twice; my first wife died of leukemia. She was cared for in a hospice in Leeds. She was 38. I was left with three kids. That was 1981. My second wife died three years ago. Breast cancer. " As for David, he was too busy raising the (seven) kids left behind to think of his own health. He had Crohn's (bowel) disease. Things went slowly at first: in 1995 he had a cholostemy. Then later an iliostemy. "It progressed into the bowel cancer. But I didn't do anything about it. It's my fault," he says, fatalistically. "If I had, this – " he gestures, weakly to himself, "probably wouldn't have happened." Things started taking a turn for the worse about a year ago, when he started having throat problems. “They thought they’d cured it, but it seems to have come back. You don’t think you’re ever going to live forever, do you?" I ask how many drugs he takes. He mumbles: "Follow me in here". He shuffles and makes his way slowly, past the myriad books he reviews, to a cramped bedroom. A huge array of pills sit on a dressing table. His bed is specially adapted, just like the ones you see in hospital. He picks up various bottles one by one. "Anti-sickness pills … morphine … E45 …." He reels off name after name. "Eye drops …" He picks up another. Then one more. "These are to keep me awake, s'new experimental drug. These are patches, slow input morphine." "It's a hospice by itself," he smiles. So how does he cope? “The worst thing is the lack of speech. When you first came,” he says, turning to his carer, “I could speak all right? I just stopped speaking. About a year ago. I can cope with all the other things. Arthritis I’ve got. Not being able to express myself as much as I’d like to [is the worst thing].” He gets annoyed when I ask if he’s suffering. “I’m not suffering, let me say. Don’t talk about suffering. It’s a bad term to use. Pain you can put up with. Speaking you can put up with. People not treating you as an average normal human being: I hate being referred to as a patient, a service user. All these are rubbish terms, they don’t mean anything … Nobody worries about your mind." How long does he think he’s got? “Two months. Three months maybe. I’m not counting the days. I’m now in minus days. They gave me 12 months eighteen months ago.” He has had two wives die; his parents; a boy who died when three. Now at the end of his own life, David says: "We don't know how to cope with death." When I ask him what nuggets of wisdom he has gleaned from his own journey, he simply replies: "I'm more concerned with living well than dying well." David died in Trinity Hospice, London, on 12 August 2009. * Mandy Mandy Paine, 46, Littlehampton, south coast of England: End-stage chronic obstructive pulmonary disease (COPD). Mandy is bloated, house-bound, her legs fattened by the steroids she is forced to take. Gazing down on her wheezing form, hooked up to an oxygen cylinder, a fading photo reveals a slim, smiling woman. She is beautiful. This is Mandy, too. A framed poem sits nearby, written for her children when she is gone. “I will be the wind in the trees...” it begins. Today, Mandy is breathless, her voice husky. Her face and features are scarred by Psoriasis. Her immune system has broken down. She suffers from severe end-stage chronic lung disease – COPD, or chronic obstructive pulmonary disease. She is slowing suffocating. Thanks to her flute training, she is able to survive on the smallest of breaths. But her lungs are dying and with it, so is she. She talks about her COPD quite openly: it is chronic, getting worse, has landed her in hospital many times – including on the edge of dying – and could kill her at any moment. She has lived with it since a girl. "I'm trying to survive … but I know I am dying. There are things I could do six months ago I can't do now. My memory's not brilliant any more. It's the drugs and the oxygen. There's the frustration of trying to find words. It's like looking through the world with net curtains. Sometimes it's like trying to claw your way through cotton wool." “I have my mask,” she says. “When I’m not coping I put my mask on. I smile, 'yeah I’m fine', whereas inside you’re screaming, shouting that 'no I’m not fine, I’m not coping, no I don’t want to do this anymore'.” She reels off the long list of drugs that keeps her alive – but with increasing ineffectiveness. A constant supply of oxygen is her lifeline. But all too often starved of that same life-giving breath, her heart beats too fast; she has angina. Other complications have arisen: She once lost all her hair during a bout of meningitis; she survived, but then suffered a stroke. “If I get something like a tummy bug, I can’t stop. And I’m on morphine for pain – that’s what nobody tells you. When you have COPD you will have pain. Sometimes it’s worse than a patient with lung cancer. Where my lungs have died off, it rubs against my muscles. It’s like a rat gnawing away at my chest … every time I breathe, every time my heart beats." Long-term drug use has eaten into her stomach. She has been vomiting blood. Her vision is going in one eye. The steroids produce cramps: she takes quinine, the anti-malarial, to offset the effects. She takes water tablets each day, too, to reduce the swelling that comes with the steroids. “Your body just swells up, absorbs fluid. You get tree trunk legs, especially if you’re sat in a wheelchair.” As a result, you have to learn to read your own illness, says Mandy. As do those around you. "Sometimes I don’t realise I’m getting very blue. My husband will say ‘I think you need to take your oxygen’. Why? ‘Because you’ve got black lips’.” He is a saint, she says. Even with him, life has not been easy. Money is tight, depression never far away. Her younger son has autism; an older son has struggled with a drug addiction. She still teaches piano, though, her cats treading carefully around its wooden legs: “That will be the last thing that I give up. It’s not for the money. It’s the thing I can still do.” That, and her strong faith keep her going. She has had close calls, she nods. “The family has been told this is it but I’ve pulled through – mainly through my own determination.” Did she remember the onset of death? “Some of it I’ve blocked out. Some of it I remember. I remember my sister by my side, telling me to breathe. And I feel sorry for her, because it’s been a strain on her life.” A terrible look of guilt washes over her tired features. “I feel a lot of frustration people have to look after me ... I should be looking after them." Like David, her friend, she opposes assisted suicide. Life is too precious. "There are other ways around it. Like I’ve done.” She reaches behind her and pulls out a sheet in a clear folder. “An advanced directive. That’s telling people I don’t want to be resuscitated. I want to be made comfortable. I don’t want a machine breathing for me. Let me go quietly. I think it’s easier for my family, when we get to the point of no return. I don’t want them turning off the machine." I notice a teddy bear. She smiles. Her face lights up and the ghost of the young woman in the photo flickers into life. "I have a whole collection," Mandy beams. "Every bear holds a memory. I can pick one up and tell you where I got it. When I go I want one of my bears to go with me. And a bell – because I'm terrified they'll stick me in a box before it's my time." Meanwhile, she lives out each day and makes the most of the time she has. "I've always tried to look ahead, rather than what's happening. I've organised my own funeral, recorded my own CD to be played, made a memory box for my kids, and written my own liturgy – because nobody knows me but me. I don't want it to be a sad occasion, I want a celebration. I don't want it to be a burden. The only thing I've left them to choose is my coffin." Then her voice runs out. Mandy has been referred to a neurological unit for the loss of vision in one eye. * Penny Penny Deacon, 33, Isle of Wight, off Southampton: Breast cancer. Penny looked well, but said she had a bad day the day before. It was the chemo. She'd sat in bed with her new TV, but it only made her feel worse. "You feel the aches and pains and know it's the cancer travelling through your body… you feel quite depressed." Despite this, an infectious smile sat permanently on her lips. The cancer which had spread, despite a double mastectomy, had done little to quell the energy, the life, which bubbled from her. She knew, though, that even with the chemotherapy she was unlikely to make two years. Without it: six months or less. She'd only been on it a week when we met. She started laughing. "I'm aiming for five years! But … it's difficult to know … how long I will last …" her voice dropped. "All the statics unfortunately for someone in my situation say not very long. But I, you know, try not to focus on that too much because I think I'd go mad." The irony for Penny was her youth: her age, her hormone levels, meant the disease spread faster around her body than a woman far older. She'd had a troubled childhood, left home at 16, yet managed to study Law and become a sergeant in the local police force. Then the cancer struck. "I first found a lump in May 2006," she said. "I was told there was only about a 10 percent chance it would ever be terminal. I had an operation to remove the lymph nodes, with six months of chemotherapy and three months of radiotherapy. I was then cancer free and felt very positive. It really didn't faze me very much. About a year later I found another lump in the other breast: that was February 2008. I then had a bit of a battle with the NHS here getting treatment – there were problems getting scans, etc. Eventually I got myself admitted to the Marsden in London [specialising in cancer care and treatment] where I ended up having a double mastectomy and reconstruction. It was mammoth surgery, nearly 12 hours. But having the reconstruction at the same time," she said, "meant at least I had some 'bumps' of some kind still left." Whilst on a skiing holiday in January this year she felt a twinge in her back. "I'll need to get it checked when we get back, I told my partner. I then had a very busy time skiing: I was hurling myself down black runs, I was having a really good time. I came back, had the scan on the 2nd February and they phoned me on the 3rd February and told me unfortunately it had travelled to four areas of my spine. That was four weeks ago now. That was when I was told it was terminal." Her body looked whole but the scans revealed a different truth: there were two tumors on her liver. A rib was cracked in three places, due to cancerous build up. She also had cancer in her left knee and in her hips. She spoke very matter-of-factly: "It's progressing around my body quite quickly." Because people knew she was dying, that too caused complications. "Some people completely avoid you, because they don't know what to say. If I am put in a situation where we have to talk, then everyone feels uncomfortable. Some people get very upset. Which makes me upset. And that makes them more upset. And then it becomes a big snotfest!" she laughed. "Some people who know me quite well make fun of my situation, which I appreciate. One friend sent me a text and said if you see a tall skinny guy dressed in black and carrying a scythe, punch him in the face and tell him to f--- off! Which really made me laugh!" One of the hardest things she'd had to do was tell her family. "You never want to tell your mum and your dad you're going to die. You can tell they want to be strong for me. But at the same time they're desperately upset. The more upset people are around me, the more upset I am. It's brought up things from the past: apologies are made, people have regrets and that pains me too. I would hate for me to leave any guilt for silly family squabbles years ago. I don't think it helps anyone really." She fell sober for a moment. "I'm still getting my head around the fact I'm terminal," she said. "Some days I wake up and think it's just not fair. I spent a long time struggling what I did career wise and emotionally a few things from my background. Now I've found a career I love; I'm in a stable relationship; I love my house; and my life seems … settled. It seems so unfair when I've worked so hard to get all of that and to have fought and remained positive throughout my first two times of being diagnosed to be told I'm going to die anyway. It seems very unfair." As a war raged in her cells, Penny busied herself preparing a charity ball. She'd already raised £20,000 for cancer charities. She was raising money for three others, "but not just cancer charities, because I didn't want to seem a bit self-obsessed." One was for the local Motor Neurone Disease Association, another a fund for relatives of police officers who died in service. "I like little events to keep me going," she said. Then, looking over the rim of her coffee cup, she looked crestfallen for one – tiny – moment. "There are days, of course, when you wake up and wish it could happen quicker. Just to be over and done with. Other days I wake up and the grass seems greener, the sky seems bluer and I want to do as many things as I possibly can. Before my time is up." She giggled and a smile lit up her face. "I suppose that's natural." Penny died on 4 April 2009. * Tina Tina Fay, 56, Lee-on-Solent, south coast of England: Motor Neurone Disease. Her words slur. Perhaps, unkindly, you would think she was a drunk. Why not? Many others have. They have thrown insults at her. Refused to serve her. Yet she is at her most lucid ever, she says. Far more so than when she was a young woman. We meet in a coffee shop on the shores of Portsmouth. She talks carefully; in fact, she has had speech therapy. You can see she was beautiful in her younger days. Her eyes catch yours and just for a moment you can see that young spirit flash within. Then you see the crutches. Tina has Motor Neurone Disease (MND). A former champion tennis instructor and fitness expert who, ironically, worked at times with the chronically-ill and dying, Tina is rapidly losing the use of her body. She fights it though – fights it hard. She has to sip from coffee and water as she struggles to speak. You can see the effort written into the wrinkles at her brow and temples. But laughter and a smile surface quickly, too, long a habit. "I was always very mad," she says over the background din. "I love fun. I just love daring sports and fun. I did a lot of diving, skiing, activity, I love active life. And parties. Just, just - oh." She stops, emotion getting the better of her. Her life now is dominated by the effects of the illness which is killing her. Most MND sufferers don't live beyond three years. She has. As Tina explains: "Stephen Hawking is the longest surviving [MND sufferer] ever. Sadly for me I have the shortest version, the one that goes the quickest. ALS it's called [Amyotrophic Lateral Sclerosis]." Is it going to kill you? "Oh, for sure. I will be lucky to get to 60 and I'm 56 now. That is my aim," she says, with a steely determination. She worked as a trainer in a gym and noticed she was tripping up a lot. It took her a few months to realise it wasn't just clumsiness. "I thought I had MS – multiple sclerosis – that was middle of 2005. And so I took myself to the doctor, my left hand at that time … I had a problem picking up things. My speech was ok then. But I took a year to be diagnosed. That's common. With Motor Neurone, there's no definitive tests: it's a process of elimination. So they eliminate everything else and that's the last thing left." The testing was not pleasant. She had an EMG to test the signal from her brain to the muscles in her body: "They put horrendous long needles into you and then you have to tense your muscles – awful. And then I had a spinal tap. And then various other electro things. And MRIs [scans], a few of them." She pauses to drink, her voice collapsing under the weight of words. "Unfortunately by then I knew a lot about it. I asked the neurologist to be plain speaking, which I prefer. I also took myself up to Kings in London for a second opinion, which is the Centre of Excellence. And they confirmed it." The disease is neurological. Simply put, the messages don't get from your brain to the muscles, and the neurones in the brain start to die. As they die the muscles wither and stop working. "It's a bit like a domino effect – that stops, and that stops, then that stops. It's very insidious really." "I'm past my sell-by-date!" she laughs. "Statistically they say you have 18 months from diagnosis. For some it's less, nine months. Two years tops. I've outlived that so far. According to them, I'm very unusual. I'm still walking, albeit awkwardly. I should really be in a wheelchair and a lot more disabled than I am. Having said that, I started off extremely fit." Eventually she will have to speak with the aid of a machine, like Hawking. Before the end comes, she won't be able to move a muscle. She will be trapped inside her own body. "It's a bummer isn't it!" she rolls her eyes. "But my brain is getting sharper. I'm so quick now." I wonder how the disease has changed her personality. "I'm totally different," she answers. "I'm not so impetuous. I am forced to think now what I do. Which is unlike me. And I think I'm a little less confident … I was always overly confident. Probably a pain in the neck type person! I was always happy. I don't have mood swings. I was always very even." Today? "Now I have to fight. I have to make myself not give in to downers. Which at times is tough. Because I can't do what I want to do." Her faith sustains her though; she was, until the end of her marriage, a Jehovah’s Witness. "I don't find it hard to talk about dying and how I am preparing," she says, although she admits it is difficult to talk about it with her two grown sons. "I think I shock people sometimes with my jesting and frankness but I am dealing with reality and don't see why people should bury their heads in the sand. After all, I can't." Tina has had a bad fall recently, and is finding mobility increasingly difficult, but says: "I'm still ok." * Greg Greg Wilford, 20, Tyne & Wear, northern England: Duchenne Muscular Dystrophy. Greg is 20. A young man at university. He likes a beer. Has plenty of mates. Studying screenwriting, he hopes one day to make it to the big screen. If he lives that long. "Most people would call it an affliction," he laughs, speaking from the electric wheelchair which is now a constant companion. "I'm a fan of Leeds United and football in general. I play – and lose – a lot of poker to my flat mates. I'm into film, music, reading – although I don't do as much as I'd like – and socialising," he chuckles, "drinking I mean, and really just trying to live a normal a life as possible." Greg is bright, ambitious, mature and very sociable. He has also suffered from Duchenne Muscular Dystrophy (DMD) since birth. He can barely move a muscle. Over time this degenerative genetic condition is erasing the protein in those same muscles, steadily weakening them. It starts in the arms and legs from infancy (the 'motor muscles'), then moves onwards into the rest of the body. "I was confined to a wheelchair at the age of nine," Greg states. "As sufferers get older, the respiratory and cardiac muscles begin to weaken, causing complications with breathing. Life expectancy ranges from early teens to mid twenties. Some people live to their thirties. The condition is incurable, but can be allievated." Three years ago he spent four months in hospital recovering from respiratory failure. It left him with a scar across his throat. He has a scar on his back from an operation that anchored a metal rod to his spine. "My heart's a bit knackered – I blame the drink!" he jokes. "But aside from that I feel fine." Daily physiotherapy is a necessity. A raft of heart medication combats cardiac difficulties. A machine helps him breathe at night. As he admits, rather matter-of-fact: "My day-to-day life requires me to have a 24-hour care assistant to aid me, for just about everything: dressing, bathing, feeding and university work." Given the nature of his condition, I wonder if his parents ever explained death to him when he was younger? "It's an interesting question you ask. I kind of see it like this: whether it was right or wrong of them to do so, my parents never tried to convince or pretend that one day something magical was going to happen and I would be 'better' for want of a more suitable word. At the time, and growing up, it was quite a strange thought at the back of my mind knowing that I would always – no matter what I do – continue to deteriorate and there's nothing I can do about it. I mean that, as you can imagine, is quite a difficult concept to get your head around, especially for a teenager." A lot of people just give up, he confesses. "A former carer of mine went to a visit a lad, 18 years old, with DMD in hospital. In the ward sitting next to him were his parents waiting at his bedside. Anyway, this carer of mine began talking about this programme he'd seen on Channel 5, about a young lad with the same condition who talked about his life, his DMD and the inevitability that he is going to die fairly young. While the carer was explaining this the lad's dad cuts him off and asks him to step outside. He tells him that their son doesn't know that he's going to die young in case it frightens him!! Now I'm not a parent of a disabled child. To me it is one of the most difficult positions for someone to be in for reasons that I'm sure are obvious; so in a way I can kind of empathise with why they would choose not to tell him. They wanted him not to worry, they wanted him to enjoy his life. And I think you'll find this is the majority of cases." "My parents on the other hand –" he starts laughing, "I think were open with me so I understood what I had to do … and what I was up against. In a way it motivated and encouraged to crack on … that in the end no matter whether I chose to lie back and wait or carry on as normal then if it happens it's still going to happen." "To put it another way," he says, "I'm going to quote the late Bill Hicks, who when confronting the fact that smokers are more likely to die due to a higher risk of contracting cancer, said: 'Here's a fact for you, non-smokers die everyday too.' Morbid a subject as death is, it happens to us all and fortunately it's something that we really can't do anything about and thus there is no point fretting about it – not when there's cider to enjoy! That's my view anyway." Greg says: "All's ok." This story was commissioned for The Times Magazine ©2009. |
|
|
You can buy this article, and seek new commissions, either by contacting me direct or my syndication agency, www.featurewell.com
|
|